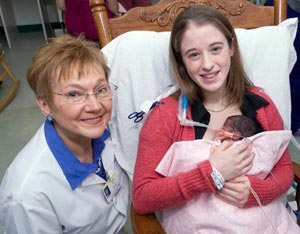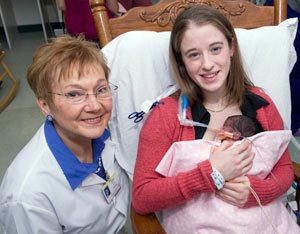 KINGSTON, R.I. – March 19, 2008 – A division of the National Institutes of Health has awarded a University of Rhode Island nursing professor a $2 million, 5-year grant to continue her investigation into the benefits of delaying umbilical cord clamping for pre-term infants.
KINGSTON, R.I. – March 19, 2008 – A division of the National Institutes of Health has awarded a University of Rhode Island nursing professor a $2 million, 5-year grant to continue her investigation into the benefits of delaying umbilical cord clamping for pre-term infants.
The National Institute for Nursing Research is funding the project, which will be conducted at Women & Infants Hospital in Providence.
The nursing research agency provided $392,000 for a smaller, earlier project involving 72 mother-infant pairs, which showed that a brief delay in clamping the umbilical cords of babies born before 32 weeks prevents bleeding in the brain and infections. The findings garnered international attention.
“That was a Phase One study, which allowed us to test the protocols and make some initial findings,” said the principal investigator, Judith Mercer, a URI clinical professor of nursing and certified nurse-midwife. “But to have delayed cord clamping become part of clinical practice in hospitals around the nation, we needed to complete larger studies.”
 “Preliminary data in support of this application has already shown that this simple and straight forward maneuver may improve neonatal outcomes,” said James F. Padbury, MD, pediatrician-in-chief at Women & Infants Hospital.
“Preliminary data in support of this application has already shown that this simple and straight forward maneuver may improve neonatal outcomes,” said James F. Padbury, MD, pediatrician-in-chief at Women & Infants Hospital.
Current obstetrical practice in the United States for very low birth weight infants is to clamp umbilical cords immediately. But Mercer said when immediate cord clamping occurs, more than 25 percent of the fetal-placental blood volume may be left in the placenta, acutely increasing vulnerability to hypovolemia, a loss of blood and fluids that can lead to shock. The earlier study showed that there were fewer cases of intraventricular hemorrhage and infection among those babies whose cords were clamped after a brief delay. Male infants showed even greater benefits from delayed cord clamping. However, the study may have been too small to find negative effects of delayed cord clamping.
“Of the approximately 57,000 infants born annually at less than 1500 grams, 10 percent develop cerebral palsy and 25 to 50 percent show later cognitive and behavioral deficits affecting school performance, with higher rates found in males,” Mercer said.
The new study will involve 212 infants to validate earlier positive findings and to identify the causes of such benefits through the study of biologic markers, including measurement of immunoregulatory proteins, circulating stem cells and red cell volume.
The infants will be selected randomly starting in April for inclusion in a control group in which cords will be clamped immediately, or an experimental group in which cord clamping will be delayed 30 to 45 seconds. In the experimental group, the infants will also be held lower than the placenta, which allows gravity to move more umbilical cord blood into the baby.
“We are going to measure the amount of stem cells in the cord blood one hour after birth and in the body 24 hours later,” Mercer said. “The theory is that if the baby gets additional cord blood, they will get more stem cells which may help prevent infection. Earlier work shows that this procedure may result in preterm babies needing fewer blood transfusions.”
Each baby will be followed until they are seven months of age, with an assessment of motor outcome planned at the conclusion.
“This low tech change in clinical practice has the potential to reduce the risk of disease and disability and to improve the neonatal and early childhood outcomes for these most vulnerable preterm infants,” Mercer said. “This area of research comes from 30 years of work as a practicing nurse-midwife. I have always delayed cord clamping in my practice with term infants.”
The nursing professor said she wants to expand her research to study the effects of delayed cord clamping and “milking” the umbilical cord (manually moving the blood from the cord to the baby) at time of caesarean section, and look at the effects of delayed cord clamping on full-term infants.
Her leadership in such research is being noted around the world. Mercer said a group of researchers in Australia is planning a large study to begin in 2009, and Mercer has been asked to serve as a consultant.
Among her collaborators for the $2 million federal study are: URI Psychology Professor Joseph Rossi of the URI Cancer Prevention Research Center, statistical consultant; URI Nursing Professor Mary Sullivan, chair of the study’s Data Safety and Monitoring Committee; and from Women & Infants Hospital, James Padbury, MD, and William Oh, MD, neonatologists; Betty Vohr, MD, development pediatrician; and Stephen Carr, MD, maternal fetal medicine specialist. Vineet Bhandar at Yale will be analyzing biological markers and Paul McMillan of Rhode Island Hospital’s Core Research Laboratory will be doing the red cell measurement.
Pictured above
Judith Mercer, URI clinical professor of nursing and certified nurse-midwife, left, with Roxanne Rodrigues and her baby Selena, in the Neonatal Intensive Care Unit at Women & Infants Hospital. Born at 26 weeks, Selena would have been eligible for Mercer’s study. URI Department of Communications and Marketing photo by Michael Salerno Photography
Also, the smaller image above links to the NBC 10 Health Check Video center where you can select the “Umbilical Cord Study, March 19” link to view the report (2:33).